Drug metabolism
DEFINITION:
The
conversion of drug into metabolites by enzymatic or non-enzymatic process
inside the body is known as biotransformation or drug metabolism.
Or
Drug metabolism is a process in which
lipid soluble drugs are converted to more water soluble products (which are not reabsorbed from kidney tubules and excreted in the urine).
EXPLANATION:
Humans are
exposed throughout their lifetime to a large variety of drugs and nonessential
exogenous (foreign) compounds (collectively referred to as xenobiotics)
that may pose health hazards.
Drugs taken for
therapeutic purposes as well as occupational or private exposure to the vapors
of volatile chemicals or solvent pose possible health risk; smoking and
drinking involve the absorption of large amounts of substances with potential
health effects. Furthermore, the ingestion of natural toxins in vegetables and
fruits, pesticides residues in food, as well as carcinogenic pyrolysis products
from fats and protein formed during the charbroiling of meat have to be
considered. Most of these xenobiotics undergo enzymatic biotransformation by
xenobiotic metabolizing enzymes in the liver and extra hepatic tissues, and are
eliminated by excretion as hydrophilic metabolites.
In some cases,
especially during oxidative metabolism, numerous chemical procarcinogens form
reactive metabolites capable of binding covalently to proteins or nucleic
acids-a critical step to mutagenicity, cytotoxicity, and carcinogenicity.
Detoxication and
toxic effects of drugs and other xenobiotics have been studied extensively in
various mammalian species. Frequently, differences in sensitivity to these
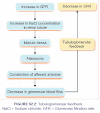
toxic effects were observed and can now be attributed to genetic differences
between species in the isoenzyme/isoforms of cytochrome P450 monooxygenases
(CYP450). The level of expression of the CYP450 enzymes is regulated by
genetics and a variety of endogenous factors such as hormones, gender, age,
disease, and the presence of environmental factors such as inducing agents.
Drugs were developed and prescribed under the old paradigm that “one dose fits
all” which largely ignores the fact that humans (adults and children) are
genetically and metabolically different, resulting in a variable response to
drugs.
Drugs can no
longer be regarded as chemically stable entities that elicit the desired
pharmacologic response and then are excreted from the body. Drugs undergo a
variety of chemical changes in the animal organism by enzymes of the liver,
intestine, kidney, lungs, and other tissues, with consequent alterations in the
nature of their pharmacologic activity, and toxicity.
Drug therapy is
becoming oriented more to controlling metabolic, genetic, and environmental
illnesses (such as cardiovascular diseases, mental illnesses, cancer, and
diabetes) than to short term therapy associated with infectious diseases. In
most cases, drug therapy lasts for months or even years and the problems of
drug toxicity from long term therapy become more serious. Therefore, a greater
knowledge of drug metabolism is becoming essential.
Metabolism plays
a central role in the elimination of drugs and other foreign compounds
(xenobiotics) from the body. Most organic compounds entering the body are
relatively lipid- soluble (lipophilic). Therefore, to be absorbed, they must
traverse the lipoprotein membranes of the lumen walls of the gastrointestinal (GI)
tract. Once in the bloodstream, these molecules can diffuse passively through
other membranes to reach various target organs to effect their pharmacologic
action. Owing to their re-absorption in the renal tubules, lipophilic compounds
are not excreted to any substantial extent in the urine.
If lipophilic
drugs or xenobiotics were not metabolized to polar, water soluble products that
are readily excretable, they would remain indefinitely in the body, eliciting
their biologic effects. Thus, the formation of water soluble metabolites not
only enhances drug elimination, but also leads to compounds that are generally pharmacologically inactive and relatively nontoxic. Consequently, drug
metabolism reactions traditionally have been regarded as detoxification
( or detoxification) process.
EFFECTS OF BIO-TRANSFORMATION REACTION ON PHARMACOLOGICAL ACTIVITIES OF DRUGS:
Biotransformation
reaction may have different effects on the pharmacological activity of the
drugs, these are;
- active drug to unactive metabolite
- active drug to more active metabolite
- unactive drug/pro-drug to active metabolite
- active drugs to reactive metabolite
Active drug to inactive metabolite:
The active drug may be converted into inactive metabolites, e.g. amphetamine
converted to phenyl lactone.
Active drug to active metabolite:
However, it is incorrect to assume that drug metabolism reactions are always detoxifying. Many drugs are bio-transformed to pharmacologically active metabolite. e.g. during demethylation, codeine is converted to morphine.Drug to active metabolite:
Some metabolites have significant activity that contributes substantially to the pharmacologic effect ascribed to the parent drug. Occasionally, the parent compound is inactive and must be converted to a biologically active metabolite. e.g. hetacillin to ampicillin by hydrolysis.Active drug to reactive metabolite:
In addition, it is becoming increasingly clear that not all metabolites are nontoxic. Indeed, many toxic side effects (e.g., tissue necrosis, carcinogenicity, teratogenicity) of drugs and environmental contaminants can be attributed directly to the formation of chemically reactive metabolites that are highly detrimental to the body. Its example is acetaminophen, which causes hepatic necrosisPATHWAYS OF DRUG METABOLISM
Drugs, plant toxins, food additives, environmental chemicals, and other chemicals foreign to the body undergo enzymic transformations that usually result in the loss of pharmacologic activity. The term detoxication describes the result of such metabolic changes. Although drug metabolism usually leads to detoxication, the process of oxidation, reduction, glucuronidation, sulfation, and other enzyme-catalyzed reactions may lead to the formation of a metabolite having therapeutic or toxic effects. This process is often referred to as bioactivation. One of the earliest examples of bioactivation was the reduction of Prontosil to the antibacterial agent sulfanilamide. Other examples of drug metabolism leading to therapeutically active drugs include the hydroxylation of acetanilide to acetaminophen, and the N-demethylation of the antidepressant imipramine to desipramine and the anxiolytic diazepam to desmethyldiazepam.The liver is the major site of drug metabolism, although other xenobiotic-metabolizing enzymes are found in the nervous tissues, kidney, lung, plasma, and the gastrointestinal tract (digestive secretions, bacterial flora, and the intestinal wall). Although hepatic metabolism continues to be the most important route of metabolism for xenobiotics and drugs, other biotransformation pathways play a significant role in the metabolism of these substances. Among the more active extrahepatic tissues capable of metabolizing drugs are the intestinal mucosa, kidney, and lung. The ability of the liver and extrahepatic tissues to metabolize substances to either pharmacologically inactive or bioactive metabolites before reaching systemic blood levels is called first pass metabolism or the presystemic first pass effect. Other metabolism reactions occurring in G.I.T. are associated with the bacterial and other micro flora of the tract.The pathways of xenobiotics metabolism have been divided into two major categories.
- phase 1 reactions
- phase 2 reactions
PHASE 1 REACTIONS (FUNCTIONALIZATION REACTION):
In these
enzymatic reactions a new functional group is introduced into the substrate
molecule, an existing functional group is modified; an acceptor site for phase
2 transfer moieties is exposed, thus making the xenobiotic more polar and
therefore more readily excreted. It includes;
a) Oxidation.
b) Reduction.
c) Hydrolysis.
OXIDATION:
In oxidation a
drug molecule is converted to its oxidized metabolite by introducing molecular
oxygen in hepatocytes involving cyto P450 monoxygenase system. Oxidation also
occurs in extra hepatic tissues by removing the hydrogen atom from the parent
drug molecule involving other enzymes like dehydrogenases.
REDUCTIVE REACTIONS:
As the name suggest “these reactions involve the addition of hydrogen atom or a pair of
electron or removal of oxygen atom from the parent drug molecule”.
Explanation:
These reactions are relatively uncommon. They mainly
occur in the liver microsomes but occasionally they also take place in other
tissues.
Reductive processes play an important role in the
metabolism of many compounds containing carbonyl, nitro and azo groups. Bio-reduction
of carbonyl compounds generates alcohol derivatives, whereas nitro and azo
reductions lead to amino derivatives. The hydroxyl and amino moieties of the
metabolites are much more susceptible to conjugation than the functional groups
of the parent compounds. Hence, reductive processes, as such facilitate drug
elimination.
Reductive pathways that are encountered less
frequently in drug metabolism include reduction of N-oxides to their
corresponding tertiary amines and reduction of sulfoxides to sulfides.
Reductive cleavage of disulfide linkages and reduction of carbon-carbon double
bonds also occur but constitute only minor pathways in drug metabolism.
Reduction
reactions are given below, these are;
i.
Reduction of Aldehydes and ketones: The carbonyl
moeity, particularly the ketone group, is encountered in many drugs. In
addition, metabolites containing aldehyde and ketone functionalities often
arise from oxidative deamination of xenobiotics (propranolol, chlorpheniramine,
amphetamine). Owing to their ease of oxidation, aldehydes are metabolized
mainly to carboxylic acids. Occasionally, aldehydes are reduced to primary
alcohols. Ketones are generally resistant to oxidations and reduced mainly to
secondary alcohol. Alcohol metabolites arising from reduction of carbonyl
compounds generally undergo further conjugation (e.g., glucuronidation)
Divers soluble
enzymes, called “aldo-keto reductases” carry out bioreduction of aldehydes and
ketone. They are found in the liver and other tissues (e.g., kidney).
ii.
Azo and Nitro Reduction: In addition to
oxidative systems, liver microsomes also contain enzyme systems that catalyze
the reduction of azo and nitro compounds to primary amines. A number of azo
compounds, such as prontosil and
sulphasalazine are converted to aromatic primary amines by azoreductase, an
NADPH-dependent enzyme system in the liver microsomes. Evidence exists for
participation of CYP450 in some reductions. Nitro compounds, for example,
chloramphenicol and nitrobenzene, are reduced to aromatic primary amines by a
nitroreductas, presumably through nitrosamine and hydroxylamine intermediates.
These reductases are not solely responsible for the reduction of azo and nitro
compounds; reduction by the bacterial flora in the anaerobic environment of the
intestine may also occur.
iii.
Miscellaneous Reductions: Several minor
reductions also occur. Reduction of N-oxides to the corresponding tertiary
amine occurs to some extent. This reduction pathway is of interest because
several tertiary amines are oxidized to form polar water soluble N-oxide
metabolites. If reduction of N-oxide metabolites occurs to a significant
extent, drug elimination would be impeded. N-oxide reduction is often assessed
by administering the pure synthetic N-oxide in vitro or in vivo and then
attempting to detect the formation of the tertiary amine. For example,
imipramine N-oxide undergoes reduction in rat liver preparations.
Reduction of sulfur
containing functional groups, such as disulfide and sulfoxide moieties, also
constitutes a minor reductive pathway.
HYDROLYSIS:
"A Hydrolysis is the process in which water is used to
split a substance into smaller particles, which would make a hydrolysis
reaction, a reaction in which water is used to split a substance into smaller
particles.
Explanation:
In general, esters and amides are hydrolyzed by
enzymes in the blood, liver microsomes, kidneys, and other tissues. Esters and
certain amides are hydrolyzed rapidly by a group of enzymes called
carboxylestrases. The more lipophilic the amide, the more favorable it is as a
substrate for this enzyme. In most cases, the hydrolysis of an ester or amide
bond in a toxic substance results in bioinactivation to hydrophilic metabolites
that are readily excreted. Some of these metabolites may yield conjugated
metabolites (i.e., glucuronides). Carboxylestrases include cholinestrase
(pseudocholinestrase), arylcarboxyestrases, liver microsomal carboxylases and other unclassified
carboxylestrases. Cholinestrase hydrolyzes choline like esters
(succinylcholine) and procain, as well as acetylsalicylic acid. Meperidine is
hydrolyzed only by liver microsmal carboxylestrases. Diphenoxylate is hydrolyzed
to its active metabolite, diphenoxylic acid, within I hour.
Hydrolysis reactions are given below, these are;
i.
Ester
hydrolysis:
ii.
Esters that are sterically hindered are hydrolyzed
more slowly and may appear unchanged in the urine. For example, approx. 50% of
a dose of atropine appears unchanged in the urine of humans. The remainder
appears to be unhydrolyzed biotransformed product.
iii.
Amide
hydrolysis:
Amides are more
stable to estrase hydrolysis than esters, and it is not surprising to find
amides excreted largely unchanged. This fact has been exploited in developing
the antiarrhythmic drug procainamide. Procaine is not useful because of its
rapid estrase hydrolysis, but 60% of a dose of procainamide was recovered
unchanged from the urine of humans, with remainder mostly N-acetylprocainamide. On the other
hand, the deacetylated metabolite of indomethacin ( a tertiary amide) is one of
the major metabolite detected in human urine. Amide hydrolysis of
phthalylsulfathiazole and succinylsulfathiazole by bacterial enzymes in the
colon releases the antibacterial agent sulfathiazole
PHASE II REACTIONS (DRUG CONJUGATION PATHWAYS)
Phase II reactions are also called conjugation
reaction. Conjugation reactions represent probably the most important
xenobiotic biotransformation reaction. Xenobiotic are usually lipophilic, well
absorbed in blood, but slowly excreted in the urine. Only after conjugation
(phase 2) reactions have added an ionic hydrophilic moiety, such as glucuronic
acid, sulfate, or glycine to the xenobiotic, water solubility increased and
lipid solubility decreased enough to make urinary elimination possible.
Mechanisms of conjugation reactions:
Two basic mechanisms are there, those are;
i.The xenobiotic (Drug) must first be activated to its
coenzyme A (CoA) thioester before reacting with the conjugating agent. The formation of the xenobiotic acyl CoA
thioester is of critical importance in intermediary metabolism of lipids as
well as intermediate and long chain fatty acids.e.g. Amino acid conjugation is
best example of this type of mechanism
Benzoic acid
(Drug) …... Benzoyl-Co-A
Benzoyl-Co-A + Glycine
(conjugating agent) …… Hippuric Acid
ii.The reaction involves the condensation of the drug
or xenobiotic (or its phase 1` product) with the activated form of conjugating
agent. e.g. sulfate conjugation.
Explanation:
The major proportion of the administered drug dose
is excreted as conjugates into the urine and bile. Conjugation reactions may be
preceded by phase 1 reactions. For xenobiotics with functional groups available
for conjugation, conjugation alone may be it’s fate. Traditionally, the major
conjugation reactions (glucuronidation and sulfation) were thought to terminate
pharmacologic activity by transforming the parent drug or phase 1 metabolite
into readily excreted ionic polar products. Moreover, these terminal
metabolites would have no significant pharmacologic activity. This long
established view changed, however, with the discovery that morphine
6-glucuronide has more analgesic activity than morphine in human and minoxidil
sulfate is the active metabolite for the antihypertensive minoxidil. For most
xenobiotics, conjugation is a detoxification mechanism.
Some compounds, however, form reactive intermediates
that have been implicated in carcinogenesis, allergic reactions, and tissue
damage. Sequential conjugation for the same substance gives rise to multiple
conjugated products. The xenobiotic can
be a substrate for more than one metabolizing enzyme. For example, different
conjugation pathways could compete for the same functional group. The outcome
is an array of metabolites excreted in the urine or feces. The reactivity of
the functional group determines all subsequent events. For example, major
conjugation reactions at the phenolic hydroxyl groups are sulfation, ether
glucuronidation, and methylation; for amino groups, acetylation sulfation,
glucuronidation; for carboxyl groups amino acid conjugation, ester
glucuronidation.
Conjugation enzymes may show stereospecificity
towards enantiomers when a racemic mixture is administered. The metabolic
pattern of the same drug administered orally and intravenously may be different
because of presystemic intestinal conjugation.
TYPES OF CONJUGATION REACTION:
There are mainly
seven types of conjugation reactions, these are;
a)
Glucuronidation
conjugation
b)
Sulfate
conjugation
c)
Aminoacid
conjugation
d)
Acetylation
e)
Methylation
f)
Gltathione
and mercapturic acid conjugation
Cyanide conjugation.incoming searches